Content uploaded by Nihal Thomas
Author content
All content in this area was uploaded by Nihal Thomas on Jul 15, 2019
Content may be subject to copyright.
ORIGINAL ARTICLE
DOES HYPERPARATHYROIDISM CAUSE PANCREATITIS? A SOUTH INDIAN
EXPERIENCE AND A REVIEW OF PUBLISHED WORK
JUBBIN J. JACOB,* MATHEW JOHN,* NIHAL THOMAS,* ASHOK CHACKO,† REKHA CHERIAN,‡ BEN SELVAN,§
ARAVINDAN NAIR§AND MANDALAM S. SESHADRI*
*Departments of Endocrinology, ‡Radiology, §Surgical Endocrinology and †Gastroentrology, Christian Medical
College and Hospital, Vellore, Tamil Nadu, India
Background: The association between pancreatic disease and primary hyperparathyroidism (PHPT) is controversial. We attempt to
suggest a causal correlation and characterize the nature of pancreatic disease in PHPT.
Methods: This study is a retrospective review of the medical records of patients who were diagnosed with PHPT and presented with
pancreatic disease between 1 May 2000 and 30 May 2005 at Christian Medical College, Vellore.
Results: During the period of 5 years, there were 1284 patients with pancreatic disease and 101 patients with PHPT admitted to our
hospital, accounting for 0.42 and 0.03%, respectively, of the total hospital inpatient admissions of 302 883. Of them, 13 patients had
both pancreatic disease and PHPT accounting for 1% of all admissions for pancreatic disease and 12% of admissions for PHPT.
Patients admitted with PHPT have a 28-fold increased risk of developing pancreatitis compared with patients admitted without
parathyroid disease. The ages of the patients ranged from 22 to 52 years with a median age of 37 years. There were 9 male and
4 female patients. The mean calcium values among patients with PHPT and pancreatic disease were significantly higher than patients
with PHPT without pancreatic involvement.
Conclusion: The data suggest a causal association between the pancreatic disease and PHPT. This may be correlated to the higher
calcium values. Until more information is available, it would be prudent to check serum calcium in all patients presenting with
unexplained pancreatic disease.
Key words: hypercalcaemia, pancreatic disease, pancreatitis, primary hyperparathyroidism.
Abbreviations: iPTH, intact parathyroid hormone levels; OFC, osteitis fibrosa cystica; PHPT, primary hyperparathyroid-
ism; SAP, serum alkaline phosphate; TCP, tropical chronic pancreatitis.
INTRODUCTION
Despite numerous case reports linking hyperparathyroidism with
pancreatic disease there seems to be a paucity of information
regarding the clinical characteristics of pancreatic disease in hyper-
parathyroidism. The initial description of the association was
described as early as 1940 when Smith and Cooke described
a patient who succumbed to acute pancreatitis correlated to hyper-
parathyroidism.
1
In 1962 Mixter et al. reported 62 cases of pancrea-
titis occurring in association with primary hyperparathyroidism
(PHPT) after reviewing the published work.
2
Subsequent reports
have focused on the development of pancreatitis in patients who are
operated on for hyperparathyroidism.
3–5
The contradictory point
was raised in 1980 when Bess et al. reviewed 1153 patients and
showed the coexistence or history of pancreatitis in only 1.5% of
patients and suggested that the association may be casual rather
than causal.
6
One possible reason for this turn could be the chang-
ing profile of PHPT in the developed countries, where symptomatic
disease remains uncommon and pancreatic disease with PHPT
extremely rare. Much later publications dealing with parathyroid
disease are hesitant to attribute a direct causal linkage between the
two and underplay the association. After the 1980s various studies
from developed countries have shown the association of pancrea-
titis with PHPT to range from 3.2 to 5.6%.
7–9
Data from other
developing countries show this association in approximately
2.5% of patients.
10,11
One centre from the northern India has reported that in 6.8% of
patients with PHPT, the disease was initially suspected because of
unexplained pancreatic disease.
12
As pancreatic disease remains
an important initial clinical presentation in the present setting, we
attempt to characterize it in patients with PHPT in terms of their
clinical presentation, biochemistry and imaging parameters.
PATIENTS AND METHODS
This study is a retrospective review of the medical records of 13
patients of a total of 101 PHPT patients who presented with
pancreatic disease at Christian Medical College, Vellore between
1 May 2000 and 30 May 2005. The medical records were
reviewed for patient characteristics and clinical details. Biochem-
ical records of all 101 patients with PHPT were retrieved from the
computerized hospital information processing system. The
patients were divided into group 1 having PHPT with pancreatic
disease and group 2 having PHPT without pancreatic disease.
J. J. Jacob MD; M. John MD, DM; N. Thomas MD, MNAMS, FRACP
(Endo); A. Chacko MD, DM; R. Cherian MD; B. Selvan MS; A. Nair MS;
M. S. Seshadri MD, PhD (Endo), FRCP.
Correspondence: Nihal Thomas, Department of Endocrinology, Christian
Medical College, Vellore, TN, India 632004.
Email: nihal_thomas@yahoo.com
Accepted for publication 1 March 2006.
ANZ J. Surg. 2006; 76: 740–744 doi: 10.1111/j.1445-2197.2006.03845.x
Ó2006 Royal Australasian College of Surgeons
The diagnosis of pancreatitis was confirmed by detection of an
increased serum amylase (>3 times the normal) and/or increased
lipase levels in the presence of upper abdominal pain. The diagno-
sis was confirmed by the presence of abnormalities on pancreatic
imaging. Other aetiologies of pancreatic disease including gall
bladder disease, microliths in bile, hypertriglyceridaemia, history
of alcohol intake, medications and abdominal trauma were sought.
The biochemical diagnosis of PHPT was made when persistent
increased calcium levels above the upper limit of normal was
associated with an increased circulating immune reactive intact
parathyroid hormone levels. The calcium values were corrected
for the serum albumin values and the results were expressed as
corrected calcium levels.
Detailed radiological reports were obtained from the
picture archiving and communicating system (General Electric–
Picture Archiving and Communicating System) and reviewed
with a radiologist.
Data were analysed using the Statistical Program for Social
Sciences (SPSS version 11.0 for Windows; SPSS, Chicago, IL,
USA). Descriptive statistics were used in most of the reviews as
the patient number was small.
RESULTS
Demography
Thirteen patients were identified from among a cohort of 101
(;13%) patients with confirmed PHPT who had clinical or ana-
tomical evidence of pancreatic disease over a period of 5 years in
our hospital. During the same period, there were 1284 admissions
for pancreatic disease out of 302 883 inpatient admissions. In 12
patients (;12%) pancreatic disease was the presenting symptom
and the initial clinical indication to make an assessment for para-
thyroid disease. One patient had pancreatic involvement in addi-
tion to severe bone disease as the presenting symptom. The
patients ranged from 22 to 52 years in age with a median age of
37 years. The median age of patients in group 2 was 43 years.
There were 9 (69%) men and 4 (31%) women among patients in
group 1. Among patients in group 2 there were 38 (43%) men and
50 (57%) women.
Clinical manifestation of pancreatic disease
The common presentation of pancreatic disease was either recur-
rent episodes of upper abdominal pain seen in 6 (46%) of the 13
patients or a single episode of acute pancreatitis seen in another 6
(46%) of these patients. One of the patients mentioned had an
episode of life-threatening acute pancreatitis requiring surgical
intervention. One patient (8%) presented with a painless chronic
pancreatitis characterized by malabsorption and secondary dia-
betes. The duration of symptoms before the diagnosis of PHPT
was made ranged from a few days to 22 years. The median period
before the diagnosis of PHPT was entertained was 6 months. Six
(46%) of the patients had more than five episodes of pain, requir-
ing an average of four hospital admissions for treatment of pain
before surgery could be undertaken for the parathyroid adenoma.
Significant weight loss was seen in five (38%) of the patients.
However, malabsorption was documented in only one patient
(8%). Other causes of pancreatitis were sought in all patients.
Nine patients (69%) had a normal gall bladder on ultrasound
imaging, whereas three (23%) had echogenic sludge in the gall
bladder and in one (8%) patient the gall bladder could not be
observed because of prior cholecystectomy. One patient (8%)
had history of chronic alcohol dependence.
Other manifestations of hyperparathyroidism
Symptomatic nephrolithiasis was seen in 6 (46%) patients in
group 1. Of the six patients with renal stones, one (8%) patient
had bilateral stone disease, one (8%) had unilateral stone disease
and four (30.8%) had nephrocalcinosis. Two patients (15%) had
a history of bone pains whereas three (23.1%) had proximal mus-
cle weakness. Two (15%) patients had a history of pathological
fractures and one (8%) patient had a palpable mass in the neck.
Among patients in group 2, bone disease was present in 60% of
patients with 28% having severe bone pains, 31% had proximal
muscle weakness, 37% had pathological fractures, 26% had radio-
logical osteitis fibrosa cystica (OFC), 13% had palpable OFC and
3% had spinal deformities at the time of presentation. Symptom-
atic renal stones were seen in 36% patients, including 16% with
the presence of renal parenchymal calcification. A palpable neck
nodule was felt in 11% of patients. The median duration of symp-
toms in group 2 patients before the diagnosis of PHPT was
24 months.
Biochemical profile
Details of the biochemical profiles of groups 1 and 2 are shown in
Table 1.
Imaging characteristics of the pancreas
The pancreatic anatomy of group 1 patients was characterized
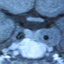
with either ultrasound or computed tomography (Fig. 1). The
details are provided in Table 2.
Localization studies and surgical outcomes
Of the eight patients who underwent ultrasound of the neck, four
(50%) had detectable lesions on the scan. A
99
technetium sesta-
mibi scan was carried out on all patients. Eleven of them had
unequivocal uptake that was suggestive of a single adenoma
and two had a doubtful uptake. Surgical details are shown in
Table 2. No postoperative complications were observed except
for transient hypocalcaemia in two of the patients operated on.
DISCUSSION
The association of primary hyperthyroidism with pancreatic dis-
ease has been controversial because of the rarity of the association
in contemporary published work in developed countries.
Table 1. Details of biochemical values in patients of group 1 and
group 2
Biochemistry Group 1
(n= 13)
Group 2
(n= 88)
P-value
Mean ± SD corrected calcium
values (mmol/L)
3.32 ± 0.52 2.97 ± 0.25 0.006
Mean ± SD fasting inorganic
phosphate values (mmol/L)
0.73 ± 0.18 0.74 ± 0.18 0.56
Mean ± SD SAP values (IU) 320 ± 296 426 ± 549 0.16
Mean ± SD iPTHvalues (ng/L) 345 ± 194 623 ± 714 0.13
iPTH, intact parathyroid hormone levels; SAP, serum alkaline phosphate.
DOES HYPERPARATHYROIDISM CAUSE PANCREATITIS? 741
Ó2006 Royal Australasian College of Surgeons
The first critical report was published by Bess et al. from Mayo
Clinic in 1980.
6
Of 1153 patients with surgically confirmed PHPT
operated on at their centre between 1950 and 1975, only 17
(1.5%) had coexisting or prior pancreatitis. This frequency
approximated the reported incidence of pancreatitis among patients
admitted to the hospital without PHPT. Other factors of possible
aetiological significance in pancreatitis, such as gallstones or
alcohol abuse, were present in 11 of the 17 patients. The rarity
of the association in their series led them to conclude that there is
no direct causal correlation between the two diseases. A later
publication from the same centre established that the majority
of patients undergoing surgery for PHPT at that centre were
asymptomatic with mild hypercalcaemia.
13
Data from hospitals
with large volume of patients with symptomatic parathyroid
disease have shown an association, which cannot be ignored.
Shepherd was the first to review this from Australia where
the association of pancreatic disease was present in 7 (5.1%) pa-
tients among the 137 who were treated for hyperparathyroidism.
7
Subsequent publications from Germany and France showed 5.6
and 3.2% of patients treated for PHPT had pancreatic disease.
8,9
Descriptive studies from Jordan, Saudi Arabia and North India, all
describe patients with pancreatic disease among proven PHPT.
10–
12
The present series shows that 12% of patients with PHPT had
pancreatic disease. During the period of 5 years, there were 1284
patients admitted with pancreatic disease and 101 patients admit-
ted with PHPT to our hospital, accounting for 0.42 and 0.03%,
respectively, of the total hospital inpatient admissions of 302 883.
Among them, 13 patients had both pancreatic disease and PHPT
accounting for 1% of all admissions for pancreatic disease. Of the
13 patients, 5 had additional possible causes for pancreatic dis-
ease. Three had gall bladder sludge, one had a history of gall-
stones requiring surgery and one patient had a history of
alcoholism. Even if these patients are to be excluded, there are
8 patients (8%) among the 101 who had no other documented
cause for pancreatic disease other than the hypercalcaemia asso-
ciated with PHPT. The calculated relative risk of having pancre-
atic disease in patients admitted with PHPT was 28 compared with
inpatients without PHPT. Similarly, the data suggest that patients
admitted with pancreatic disease have 33-fold increased chances
of having PHPT compared with patients admitted with non-
pancreatic disease. Therefore, we suggest that there is a significant
association between the two disorders.
Characterization of the pancreatic disease in
hyperparathyroidism
In the present series, PHPT presents as pancreatic disease in much
younger patients compared with the median age of presentation in
isolated PHPT. The sex distribution also shows a male preponder-
ance with the male : female ratio being almost 2:1. This is in
contrast to the female preponderance we see in PHPT without
associated pancreatic disease. In the largest series of patients with
PHPT and pancreatic disease, over 40 patients were identified
among 1224 patients operated for PHPT over a period of
30 years.
9
Among them, the mean age in patients with pancreatitis
and PHPT was 52.5 compared to 55.5 in patients with PHPT
without pancreatic disease. The male : female ratios were 1.1:1
and 0.34: 1, respectively.
Table 2. Details of patient and imaging characteristics and operative findings in group 1
Patient characteristics Imaging characteristics Operative findings
nAge Sex Size Intra-parenchymal
calcification
Ductal
calculi
Main
pancreatic
duct
Peri-pancreatic
collection
Operated Localization of
the adenoma
1 52 F Normal No No Normal No Yes Right lower
2 40 M Enlarged No No Dilated No Yes Left lower
3 45 M Enlarged Yes No Normal Single Yes Left lower
4 38 F Enlarged Yes Yes Not known Single Yes Right lower
5 34 M Normal No No Normal No Yes Left lower
6 30 M Enlarged No No Dilated No Yes Ectopic
7 22 M Normal No No Normal No Yes Left lower
8 38 F Enlarged Yes Yes Dilated Single No NA
9 35 M Enlarged Yes Yes Dilated Single Yes Right lower
10 37 M Enlarged No No Normal No No NA
11 45 F Enlarged Yes Yes Not known No Yes Left lower
12 35 M Enlarged No No Normal Single Yes Left lower
13 47 M Enlarged No No Normal No Yes Left upper
F, female; M, male; NA, not applicable.
Fig. 1. Computed tomography scan of the abdomen showing bulky
pancreas with dilated main pancreatic duct, intraparenchymal calci-
fication and intraductal calculi (arrow).
742 JACOB ET AL.
Ó2006 Royal Australasian College of Surgeons
The commonest manifestation of pancreatic disease with PHPT
is the history of recurrent upper abdominal pain (50%). In the
majority, the pancreatic origin of the disease is clarified once
serum amylase or serum lipase levels are obtained. The mean
duration of symptoms before the patients were found to have
PHPT ranged from 6 months to 22 years. The median time before
a diagnosis could be established was 24 months. Patients had, on
an average, four hospitalizations and over 10 episodes of pain
before the underlying hypercalcaemia was identified. This delay
in the diagnosis could have been avoided if calcium values were
checked in all patients with unexplained pancreatic disease at the
first instance.
In 1966, Pyrah et al. had attempted to summarize the circum-
stances under which pancreatic disease was found in association
with PHPT.
14
Modifying this, we can classify presentation of
pancreatic disease in PHPT into four important classes:
dPHPT presenting as acute pancreatitis
dPHPT presenting as acute recurrent pancreatitis with no evi-
dence of chronic pancreatitis
dPHPT presenting as chronic pancreatitis with or without
pancreatic calcification
dPHPT complicated by acute pancreatitis in the postoperative
period
We reviewed the clinical presentation in 87 patients from five
case series including 13 patients from the present series (Table 3).
Class 1 presentation was the most common, occurring in over
44% of patients, underlining the need to check calcium values
in all patients presenting with the first episode of pancreatitis. We
did not have any documented reports of patients who developed
acute pancreatitis in the postoperative period. In over one-third of
the patients the disease was more insidious and presented with
evidence of chronic pancreatitis. Parathyroid surgery at this point
may not reverse the pancreatic pathology and long-term therapy
for exocrine and endocrine pancreatic insufficiency may be
required. However, it would be still be prudent to check serum
calcium levels in these patients as early parathyroid surgery
would prevent associated renal and bone disease.
Hypercalcaemia as the mediator of pancreatic injury in PHPT
In animal models acute pancreatitis has been induced, when a two-
fold increase in serum ionized calcium was obtained by either
bolus injections or by continuous infusion of calcium.
16
Patholog-
ical changes of early acute pancreatitis with hypercalcaemia has
been observed in several animal species.
17,18
It was shown that
hypercalcaemia induced a secretory block and accumulation of
digestive zymogens within the pancreatic acinar cells.
19
In
humans, development of acute pancreatitis has been linked to
the use of therapeutic i.v. calcium administration. Among patients
undergoing cardiac surgery, evidence of pancreatic injury was
seen in 27% of patients. Although ischaemia secondary to hypo-
perfusion is considered to be the cause of this complication, the
administration of large doses of calcium chloride was an independ-
ent predictor of pancreatic cellular injury.
20
The molecular mechanism of hypercalcaemia-mediated pan-
creatic injury has still not been elucidated and remains a matter
of conjecture. We know that the earliest abnormalities of acute
pancreatitis arise within the acinar cells and that calcium is a vital
intracellular second messenger in the acinar cell for initiating
enzyme release through phosphorylation cascades. The cytoplas-
mic concentration of calcium is tightly regulated.
21
Sustained
levels of acinar cytoplasmic calcium may cause damage to the
acinar cells by the unopposed activation of zymogens, including
trypsinogen.
20
Various factors, including alcohol abuse, ductal
hypertension, ischaemia, hyperlipidaemia, viral infections and
hypercalcaemia may trigger acute pancreatitis by increasing intra-
cytoplasmic calcium levels. In the present series all patients had
corrected serum calcium above the normal range (normal levels;
2.07–2.60 mmol/L). The mean calcium values were significantly
higher among patients with PHPT and pancreatic disease com-
pared with patients with PHPT without pancreatic involvement.
This suggests that the mechanism of development of pancreatic
disease in PHPT is correlated to the hypercalcaemia. These obser-
vations suggest that hypercalcaemia per se, in addition to being an
independent risk for the precipitation of pancreatic cellular injury,
could also augment pancreatic disease in patients with ongoing
pancreatic injury because of other causes.
In the present series we have shown a higher association of
PHPT and pancreatic disease than any previous series. We postu-
late two possible reasons for this. First, parathyroid disease in the
present study is a largely symptomatic disease similar to the pre-
sentation of PHPT seen in the last century in the West. That could
account for a higher percentage of patients having associated
pancreatic disease.
Second, unusual pancreatic diseases like tropical chronic pan-
creatitis (TCP), a form of chronic calcific non-alcoholic pancrea-
titis are a common cause of chronic pancreatitis at our centre. The
exact aetiopathogenetic mechanisms of TCP remain elusive, but it
has been suggested that various factors like malnutrition, dietary
toxins and familial and genetic factors contribute to the develop-
ment of the disease.
22
We propose that the presence of hypercal-
caemia correlated to PHPT among patients susceptible to TCP
may cause an unmasking of preclinical and subclinical diseases.
The presence of large intraductal calculi similar to that seen in
TCP in 30% of patients in our series may point to that possibility.
A combination could account for the frequency of the association.
Eleven of the 13 patients underwent parathyroid surgery. Most
of the tumours (excluding one) were situated in the lower part of
the neck of operated patients. Long-term follow up was available
only in a limited number of patients. The natural history of
chronic pancreatitis correlated to PHPT is still not clear as most
patients had a limited follow up.
Table 3. Details of presentation of pancreatic disease in PHPT from four other case series in the published work
Bess
et al.
6
(n= 17)
Sitges-Serra
et al.
15
(n= 10)
Shepherd
et al.
7
(n=7)
Carnaille
et al.
9
(n= 40)
Present
series
(n= 13)
Total
(n= 87)(%)
Class 1 8 6 4 18 3 39 (44.8%)
Class 2 — 1 2 8 3 14 (16.1%)
Class 3 7 3 — 14 7 31 (35.6%)
Class 4 2 — 1 — — 3 (3.4%)
DOES HYPERPARATHYROIDISM CAUSE PANCREATITIS? 743
Ó2006 Royal Australasian College of Surgeons
CONCLUSIONS
The present study suggests a causal association between the pan-
creatic disease and PHPT. The frequency of the disease in our
setting probably correlates to the large number of symptomatic
PHPT that we see in our country. We propose that other undefined
factors that predispose our patients to tropical pancreatitis may
also unmask subclinical/preclinical pancreatic disease early in the
course of PHPT. The disease is more common in younger indi-
viduals with a male preponderance. The disease is correlated to
higher calcium values in PHPT. The exact cellular mechanism by
which hypercalcaemia causes pancreatic injury in PHPT remains
to be elucidated. Until more information is available, it would be
prudent to check serum calcium in all patients presenting with
unexplained pancreatic disease.
REFERENCES
1. Smith FB, Cooke RT. Acute fatal hyperparathyroidism. Lancet
1940; ii: 560–61.
2. Mixter CG Jr, Keynes WM, Cope O. Further experience with
pancreatitis as a diagnostic clue to hyperparathyroidism. N. Engl
J. Med. 1962; 266: 265–72.
3. Dubost CI, Jehanno CL, Poirier A, Duranteau A. [Is there a risk
of acute pancreatitis after parathyroidism?] Nouv. Presse Med.
1980; 9: 3281. (In French.)
4. London NJM, Lloyd DM, Pearson H, Neoptlemos JP, Bell PRF.
Pancreatitis after parathyroidectomy. Br. J. Surg. 1986; 73: 766–7.
5. Reeve TS, Delbridge LW. Pancreatitis following parathyroid sur-
gery. Ann. Surg. 1982; 195: 158–62.
6. Bess MA, Edis AJ, von Heerden JA. Hyperparathyroidism and
pancreatitis. Chance or a causal association? JAMA 1980; 243:
246–7.
7. Shepherd JJ. Hyperparathyroidism presenting as pancreatitis or
complicated by postoperative pancreatitis. Aust. N. Z. J. Surg.
1996; 66: 85–7.
8. Koppelberg T, Bartsch D, Printz H, Hasse C, Rothmund M. [Pan-
creatitis in primary hyperparathyroidism (pHPT) is a complica-
tion of advanced pHPT.] Dtsch. Med. Wochenschr. 1994; 119:
719–24. (In German.)
9. Carnaille B, Oudar C, Pattou F, Combemale F, Rocha J, Proye C.
Pancreatitis and primary hyperparathyroidism: forty cases. Aust.
N. Z. J. Surg. 1998; 68: 117–19.
10. Bismar HA, El-Bakry AA. Primary hyperparathyroidism. Saudi
Med. J. 2003; 24: 1214–18.
11. Younes NA, Al-Trawneh IS, Albesoul NM, Hamdan BR, Srou-
jieh AS. Clinical spectrum of primary hyperparathyroidism.
Saudi Med. J. 2003; 24: 179–83.
12. Agarwal A, George RK, Gupta SK, Mishra SK. Pancreatitis in
patients with primary hyperparathyroidism. Indian J. Gastroen-
terol. 2003; 22: 224–5.
13. Russell CF, Edis AJ. Surgery for primary hyperparathyroidism:
experience with 500 consecutive cases and evaluation of the role
of surgery in asymptomatic patients. Br. J. Surg. 1982; 69:
244–7.
14. Pyrah LN, Hodgkinson A, Anderson CK. Primary hyperparathy-
roidism. Br. J. Surg. 1966; 53: 245–316.
15. Sitges-Serra A, Alonso M, De Lecea C, Gores P, Sutherland D.
Pancreatitis and hyperparathyroidism. Br. J. Surg. 1988; 75:
158–60.
16. Mithofer K, Fernandez-del Castillo C, Frick TW, Lewandrowski
KB, Rattner DW, Warshaw AL. Acute hypercalcemia causes
acute pancreatitis and ectopic trypsinogen activation in the rat.
Gastroenterology 1995; 109: 239–46.
17. Frick TW, Hailemariam S, Heitz PU, Largiader F, Goodale RL.
Acute hypercalcaemia induces acinar cell necrosis and intraduc-
tal precipitates in the pancreas of cat and guinea pig. Gastroen-
terology 1990; 98: 1675–81.
18. Frick TW, Wiegand D, Bimmler D, Fernandez-del Castillo C,
Rattner DW, Warshaw AL. A rat model to study hypercalcemia-
induced pancreatitis. Int. J. Pancreatol. 1994; 15: 91–6.
19. Frick TW, Mithofer K, Fernandez-del Castillo C, Rattner DW,
Warshaw AL. Hypercalcemia causes acute pancreatitis by pan-
creatic secretory block, intracellular zymogen accumulation and
acinar cell injury. Am. J. Surg. 1995; 169: 167–72.
20. Fernandez-del Castillo C, Harringer W, Warshaw AL et al. Risk
factors for pancreatic cellular injury after cardiopulmonary
bypass. N. Engl J. Med. 1991; 352: 382–7.
21. Ward JB, Petersen OH, Jenkins SA, Sutton R. Is an elevated
concentration of acinar cytosolic free ionized calcium the trigger
for acute pancreatitis? Lancet 1995; 346: 1016–19.
22. Barman KK, Premalatha G, Mohan V. Tropical chronic pancre-
atitis. Postgrad. Med. J. 2003; 79: 606–15.
744 JACOB ET AL.
Ó2006 Royal Australasian College of Surgeons