Access to this full-text is provided by Wiley.
Content available from Case Reports in Otolaryngology
This content is subject to copyright. Terms and conditions apply.
Case Report
Unilateral Maxillary Sinus Actinomycosis with
a Closed Oroantral Fistula
Jason E. Cohn,1,2 Mark Lentner,1,2 Hui Li,3and Matthew Nagorsky2
1Department of Otolaryngology-Head and Neck Surgery, Philadelphia College of Osteopathic Medicine, Philadelphia, PA, USA
2Department of Otolaryngology-Head and Neck Surgery, Drexel University College of Medicine, Philadelphia, PA, USA
3Department of Pathology and Laboratory Medicine, Drexel University College of Medicine, Philadelphia, PA, USA
Correspondence should be addressed to Jason E. Cohn; jasoncoh@pcom.edu
Received 12 November 2016; Revised 20 February 2017; Accepted 27 February 2017; Published 2 March 2017
Academic Editor: Rong-San Jiang
Copyright © Jason E. Cohn et al. is is an open access article distributed under the Creative Commons Attribution License,
which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Actinomycosis is a bacterial infection due to Actinomyces israelii, a gram-positive, anaerobic organism that normally aects the
cervicofacial region. However, facial injury or trauma (i.e., dental procedures) can allow this bacteria to inhabit other regions.
ere have been rare reports of actinomycosis of the paranasal sinuses. We present a case of a -year-old female who originally
presented with a suspected oroantral stula who subsequently was found to have actinomycosis involving her right maxillary sinus.
Additionally, the dental extraction site revealed no connection with the maxillary sinus. We discuss the diagnostic approach and
management of this patient as it relates to the limited existing literature.
1. Introduction
Actinomycosis is a bacterial infection due to Actinomyces
israelii, a gram-positive anaerobic organism. Actinomyces
normally exists in the aerodigestive ora and only crosses
mucosal surfaces by means of facial injury or trauma []. Most
commonly, this will occur as a result of a dental procedure,
such as extraction or dental implants []. Actinomycosis usu-
ally occurs in regions: cervicofacial, thoracic, abdominal,
and genital []. Most cases present as a cervicofacial draining
sinusnearthemandible[].Rarely,aninfectioncaninvolve
thenoseandparanasalsinuses.Mostcommonlyyouwill
see the maxillary sinus involved; however, you can also see
ethmoid and sphenoid sinus involvement [].
2. Case Report
A -year-old female presented with right facial pain and ten-
derness since a dental extraction. Two weeks before she had
her right upper molar extracted. Shortly aer this procedure,
she began draining foul-smelling and tasting green mucus.
She also described mild right facial swelling and right maxilla
numbness, as well as right ear fullness, pressure, and hearing
loss. She denied fevers and chills. On examination, her right
maxilla was tender to palpation and there was granulation
tissue at the level of the right upper molar. However a distinct
oroantral stula was not appreciated. On nasal endoscopy,
greenmucuswasvisualizedattherightostiomeatalcomplex.
At this time, she was advised to have a CT scan of the
sinuses to further evaluate her sinus disease. CT scan of the
sinuses demonstrated complete opacication of the right
maxillary sinus with so tissue extending through the
ostiomeatal complex and into the right nasal cavity (Figure ).
erewasalsomucosaldiseaseintherightethmoid,frontal,
and sphenoid regions. ere was no le-sided sinonasal dis-
ease. Previously, the patient was treated with several courses
of antibiotics with her primary care physician and, how-
ever, still experienced symptoms. At this point, she was
broughttotheoperatingroomforrightfunctionalendo-
scopic sinus surgery (FESS) with possible closure of an
oroantral stula.
Intraoperatively, she was found to have yellow-green
mucopurulent material and edema in theright middle meatus
extending to the nasopharynx. ere was no visible disease
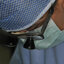
on the le side. Palpation of the dental extraction site
revealed no opening into the maxillary sinus (Figure ). e
Hindawi
Case Reports in Otolaryngology
Volume 2017, Article ID 7568390, 3 pages
https://doi.org/10.1155/2017/7568390
Case Reports in Otolaryngology
F : A coronal CT image demonstrating complete opacica-
tion of the right maxillary sinus with so tissue extending through
the ostiomeatal complex and into the right nasal cavity.
F : Intraoperative palpation of the dental extraction site
revealing no opening into the maxillary sinus (oroantral stula).
patient underwent a right middle turbinectomy, maxillary
antrostomy, and anterior and posterior ethmoidectomy. e
specimens taken from the right maxillary sinus were irregular
fragments of pink-tan brous so tissue measuring . ×.
×. centimeters (cm) in aggregate. Yellow-green mucopus
expressed from the right maxillary sinus was collected for
aerobic and anaerobic culture. Shortly aer the procedure,
the microbiologist indicated that the intraoperative anaerobic
culture revealed gram-positive, rod-shaped bacteria with
fungus-like branching of hyphae. ese rare ndings were
consistent with Actinomyces.However,thepathologyspec-
imens did not show any presence of Actinomyces.eonly
histologic nding was chronic inammation and thicken-
ing of the basement membrane in the respiratory mucosa
(Figure ).
F : A histologic specimen of respiratory mucosa with thick-
ened basement membrane and mild chronic inammation.
F : A postoperative coronal CT image demonstrating well-
aerated right maxillary and ethmoid sinuses without mucosal
thickening with a patent ostiomeatal complex aer right maxillary
antrostomy, middle turbinectomy, and anterior and posterior eth-
moidectomy.
Treatment of actinomycosis involves surgical debride-
ment as well as long-term antibiotic therapy, typically peni-
cillin []. erefore, this patient underwent FESS as well
as treatment with long-term antibiotics. In the immediate
postoperative period, the patient was seen weekly for nasal
endoscopy with debridement on three separate occasions
and was treated with penicillin-VK milligrams (mg) four
times per day. However, this therapy was discontinued early
aer a total of weeks treatment due to gastrointestinal
upset and dizziness. ree weeks aer the penicillin was
discontinued, the patient began to experience right maxillary
sinus pressure again. At this time, the patient was reevaluated
by our surgical team as well as an infectious disease specialist.
Doxycycline mg twice a day was instituted and has
continued to date. Currently, she is doing well with no
active sinonasal disease. She no longer reports sinus pressure
or drainage. On nasal endoscopy, her right ostiomeatal
complex is widely patent without mucopurulent drainage. A
postoperativeCTscanrevealedanormalmaxillaryantrum
without uid collection or mucosal thickening (Figure ).
Case Reports in Otolaryngology
3. Discussion
Actinomycosis of the paranasal sinuses was rst described
byPonckinandthenspecicallyinthemaxillary
sinus by Stanton in []. Actinomycosis of the paranasal
sinuses remains rare and has only been further demonstrated
by a small number of case reports. Occasionally, patients
can become susceptible to invasive sinonasal actinomycosis
and present with headache, visual changes, and cranial nerve
palsy [, ].
It has been shown that the presence of an oroantral
stula can predispose one to actinomycosis of the paranasal
sinuses [, ]. Our patient was originally referred to our
group for an oroantral stula. However, examination in the
oce as well as the operating room revealed spontaneous
closure of the stula. Despite this nding, sinonasal cultures
revealed growth of Actinomyces. erefore, it is important
to consider additional etiologies for actinomycosis in this
patient. For example, it has been shown that sinus hypoxia
can occur through blockage of sinus ostia causing an anaer-
obic environment for Actinomyces [, ]. is patient had
signicant edema surrounding her middle meatus; therefore
this theory is plausible. Overall, this patient demonstrated
both mechanisms of pathophysiology. e patient rst expe-
rienced odontogenic sinusitis from the penetration of oral
pathogensintothesinonasalcavitiesviaanoroantralstula.
Once this stula closed, Actinomyces was able to ourish in
an anaerobic environment due to local tissue hypoxia from
paranasal sinus inammation.
e diagnosis of actinomycosis is accomplished with a
thorough history and physical examination, the presence of
yellow sulphur granules on specimens, and specic ndings
on radiographic imaging []. CT ndings suggestive of acti-
nomycosis include opacication, unilateral lesion, mucosal
thickening, thickening of bone walls, focal areas of bone
destruction (especially of the medial wall), and calcica-
tions []. is case was unusual because of the pathogen
isolated and the lack of several typical radiologic features.
e CT clearly demonstrated right-sided opacication of all
paranasal sinuses, so tissue occupying the right nasal cavity,
and right paranasal sinus mucosal thickening (particularly
in the maxillary sinus). However, thickening of bone walls,
focal areas of bone destruction, and calcications were not
seen. Based upon the clinical course of this patient, we
recommend the usual -month treatment with penicillin-VK
mg four times per day. However, prescribing physicians
should be aware that there are potential side eects and poor
patient compliance due to frequent dosing. is patient is
improving signicantly with doxycycline; therefore, that is a
viable option. Due to the improvements seen both clinically
and radiologically, we did not feel the need to order further
testing such as magnetic resonance imaging (MRI). However,
MRI can be useful to clinicians to evaluate so tissue invasion
[].
Conflicts of Interest
e authors declare that they have no conicts of interests.
References
[]H.-J.Woo,C.H.Bae,S.-Y.Song,Y.S.Choi,andY.-D.Kim,
“Actinomycosis of the paranasal sinus,” Otolaryngology—Head
and Neck Surgery,vol.,no.,pp.–,.
[] M. Roth and K. T. Montone, “Actinomycosis of the paranasal
sinuses: a case report and review,” Otolaryngology—Head and
Neck Surgery,vol.,no.,pp.–,.
[]R.Wadhera,S.P.Gulati,A.Garg,A.Ghai,andS.Kumar,
“Frontal sinus actinomycosis presenting as osteomyelitis of
frontal bone,” Otolaryngology—Head and Neck Surgery,vol.,
no. , pp. –, .
[]N.Vorasubin,A.W.Wu,C.Day,andJ.D.Suh,“Invasive
sinonasal actinomycosis: case report and literature review,”
Laryngoscope,vol.,no.,pp.–,.
[] R.Rastogi,D.Rao,G.N.Suma,S.Bhargava,V.Rastogi,and
K. Rastogi, “Radiological features in actinomycosis of paranasal
sinus region and base of skull with oro-antral stula,” Journal
International Medical Sciences Academy,vol.,no.,pp.–
, .
[]M.B.Stanton,“Actinomycosisofthemaxillarysinus,”e
Journal of Laryngology & Otology, vol. , no. , pp. –,
.
[] G. L. Fadda, M. Gisolo, E. Crosetti, A. Fulcheri, and G. Succo,
“Intracranial complication of rhinosinusitis fromact inomycosis
of the paranasal sinuses: a rare case of abducens nerve palsy,”
Case Reports in Otolaryngology, vol. , Article ID ,
pages, .
[] A. Gannepalli, B. K. Ayinampudi, P. V. Baghirath, and G. V.
Reddy, “Actinomycotic osteomyelitis of maxilla presenting as
oroantral stula: a rare case report,” Case Reports in Dentistry,
vol. , Article ID , pages, .
[] J. H. Damante, E. Sant’Ana, C. T. Soares, and C. R. Moreira,
“Chronic sinusitis unresponsive to medical therapy: a case of
maxillary sinus actinomycosis focusing on computed tomogra-
phy ndings,” Dentomaxillofacial Radiology,vol.,no.,pp.
–, .
Content uploaded by Jason Cohn
Author content
All content in this area was uploaded by Jason Cohn on Apr 22, 2017
Content may be subject to copyright.