Available via license: CC BY-NC 3.0
Content may be subject to copyright.
© 2016 Goder et al. This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php
and incorporate the Creative Commons Attribution – Non Commercial (unported, v3.0) License (http://creativecommons.org/licenses/by-nc/3.0/). By accessing the work you
hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission
for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms (https://www.dovepress.com/terms.php).
OncoTargets and Therapy 2016:9 4793–4796
OncoTargets and erapy Dovepress
submit your manuscript | www.dovepress.com
Dovepress 4793
CASE REPORT
open access to scientific and medical research
Open Access Full Text Article
http://dx.doi.org/10.2147/OTT.S113724
Cutaneous basal cell carcinoma arising within
a keloid scar: a case report
Maya Goder1,*
Rachel Kornhaber2,*
Daniele Bordoni3
Eyal Winkler1
Josef Haik1
Ariel Tessone1
1Department of Plastic and
Reconstructive Surgery, Sheba Medical
Center, Tel Hashomer, Israel; 2School
of Health Sciences, Faculty of Health,
University of Tasmania, Sydney,
NSW, Australia; 3Department of
Sen olo gy, Osp eda le San ta Maria della
Misericordia Urbino, Urbino, Italy
*These authors contributed equally
to this work
Abstract: Basal cell carcinomas (BCCs) are one of the most frequent cutaneous malignancies.
The majority of BCCs are reported to occur on the auricular helix and periauricular region due
to ultraviolet light exposure. Despite the frequency of BCCs, those that develop within scar
tissue are rare, and the phenomenon of keloid BCCs has rarely been reported in the literature.
Keloid collagen within BCCs is associated with morphoeiform characteristics, ulceration, or
necrosis. Extensive keloid collagen is often seen in BCCs of the ear region, a site prone to keloid
scarring. This article presents a rare case of a secondary tumor (BCC) which arose on top of a
primary tumor (keloid scar) on the right auricle region in a healthy 23-year-old female after an
ear piercing 2 years prior. To our knowledge, the tumor described in this case, in contrast to
keloidal BCCs, has never been reported in the literature.
Keywords: basal cell carcinoma, BCC, keloid scar, auricle, methylprednisolone acetate
Introduction
Basal cell carcinomas (BCCs) develop within the basal cell layer of the epidermis.1
They are one of the most frequent skin malignancies2,3 accounting for 75%–80% of
all skin cancers, with 70%–80% of all BCCs occurring in the head and neck region.1
Furthermore, they are the most common type of malignancy of the ear.4 The majority
of BCCs are reported to occur on the auricular helix and periauricular region due to
exposure to ultraviolet light4 and may infiltrate the cartilage.4 Reports of an etiologi-
cal relationship between prior trauma/scar tissue and the development of a BCC have
been reported within the literature.3 To date, only five case reports of keloidal BCCs
have been discussed in the literature.5–9 Keloid collagen within BCCs is reported to
be associated with morphoeiform characteristics, ulceration, or necrosis, with exten-
sive keloid collagen seen in BCCs of the ear region, a site prone to keloid scarring.10
However, presented here, to our knowledge, is the first reported case of a secondary
tumor (BCC) which arose on top of a primary tumor (keloid scar) on the right auricle
region in a healthy 23-year-old female after an ear piercing 2 years prior.
Case report
A 23-year-old female presented with ongoing management of a keloid scar on her right
auricle with no relevant medical history. At 21 years of age, she had her ear pierced and
developed a local infection that was treated initially with topical antibiotics. Subsequently,
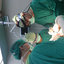
a keloid scar began to form (Figure 1). At first presentation, the lesion was observed to
be a 1 cm red keloid scar on the mid-helix of the right auricle. Initially, 40 mg of methyl-
prednisolone acetate was injected locally and she was given a prescription for a pressure
earing. Mechanical pressure is often used as a means to prevent or treat keloid scars.11
Correspondence: Maya Goder
Department of Plastic and Reconstructive
Surgery, Sheba Medical Center,
Tel Hashomer, Emek HaEla St 1,
52621, Ramat Gan, Israel
Tel +972 52 888 1555
Email maya.b.h@gmail.com
Journal name: OncoTargets and Therapy
Article Designation: Case report
Year: 2016
Volume: 9
Running head verso: Goder et al
Running head recto: Cutaneous basal cell carcinoma arising within a keloid scar
DOI: http://dx.doi.org/10.2147/OTT.S113724
OncoTargets and Therapy downloaded from https://www.dovepress.com/ on 11-Feb-2023
For personal use only.
Number of times this article has been viewed
This article was published in the following Dove Press journal:
OncoTargets and Therapy
2 August 2016
OncoTargets and Therapy 2016:9
submit your manuscript | www.dovepress.com
Dovepress
Dovepress
4794
Goder et al
At 1 month follow-up, during which time she had been
wearing the pressure earing consistently, a slight improve-
ment was observed with a mild reduction in the overall size
of the keloid scar. Another injection of 40 mg methylpred-
nisolone acetate was given locally (Figure 2).
Four months after commencing the initial treatment, the
patient presented again, and a 15% improvement was observed
with a reduction in the size of the keloid scar tissue to a diameter
of 11 mm. Again, the patient received another local injection
of methylprednisolone acetate, but at a reduced dose of 20 mg.
At 5 months follow-up, the base of the keloid was unchanged
and remained at 11 mm. However, the overall volume of the
keloid had a flattened appearance as a result of the pressure
earing. Again, the patient was administered another injection
(locally) at the original dose of 40 mg methylprednisolone
acetate. A further 10 weeks on, the base of the keloid scar
measured 10 mm and its height was reduced, with the total
thickness of the right helix of the involved area measuring
8 mm as opposed to 7 mm in the opposite ear. Of significance,
it was noted that part of the normal tissue in the involved area
was replaced by the keloid over 1 mm thickness. The dose of
40 mg methylprednisolone acetate was once again injected
locally, in conjunction with the pressure earring (Figure 3).
A further 2 months on, the base of the keloid remained
unchanged at 10 mm; however, the total thickness of the helix
reduced to 7 mm. The posterior region of the helix remained
a small flat patch, while the anterior of the helix presented
with only minimal keloid content. At this time, another injec-
tion of 40 mg methylprednisolone acetate was administered.
After completing a year’s treatment with methylprednisolone
Figure 1 Keloid scar at rst presentation.
Figure 2 Follow-up after 1 month of wearing the pressure earing.
Figure 3 Keloid scar 5 months since the initial presentation with a attened
appearance.
Powered by TCPDF (www.tcpdf.org)
OncoTargets and Therapy 2016:9 submit your manuscript | www.dovepress.com
Dovepress
Dovepress
4795
Cutaneous basal cell carcinoma arising within a keloid scar
acetate and 3 years after the original piercing, the keloid
scar became active again, appearing red and telangiectasic.
A final local injection of 60 mg methylprednisolone acetate
was administered, resulting in no improvement with a further
rapid growth in size (Figure 4).
It was decided to surgically excise the keloid lesion using
wide margins, and subsequently, the growth was sent for his-
tological examination. Histological examination determined
that the lesion was consistent with keloid and had tiny foci
of BCC arising from within. The patient provided informed
written consent for the described procedures and the use of
digital photography for the purposes of treatment, teaching
and use in academic publications.
Discussion
The first known description of keloid was found in Smith
Papyrus derived from ancient Egypt circa 3000 BC.12 The
term keloid derives from the Greek word cheloid, chele
(ηλη) meaning a crab’s claw and the suffix-oid, meaning
like.4 Keloids are benign dermal fibroproliferative tumors13
that develop after the dermis experiences local trauma
such as surgery, burns, laceration, tattoos, and infections.14
However, abnormal scarring remains poorly understood and
is a consequence of surgical and traumatic wounds.15 Keloids
are reported to be more frequent in certain ethnic groups and
has an incidence of 15%–20% in the black population.16 Fur-
thermore, these unique scars have been reported in patients
with hereditary connective tissue disorders such as Ehlers–
Danlos syndrome, in which keloids manifest as one of the
clinical indicators.17 Keloid scar may develop anywhere;
however, the ear is a common site for keloid formation, and
the scar usually occurs after trauma or ear piercing,18 although
there is limited data available for the treatment of helical rim
keloids.19 The ear is reported to be a region with a propensity
for the development of keloidal BCCs and is a site that is
prone to the development of keloids in certain individuals.10,18
This may be related to the frequent piercing of earlobes and
the trauma and infection that can often ensue.
Requena et al5 described a keloidal BCC for its striking and
distinctive features, and from a clinical pathological basis, as a
variant of a BCC deemed to be rare.10 However, this description
has been refuted by others10 with a study identifying that keloid
BCCs are not as rare as originally stated and therefore do not
characterize a distinctive clinicopathological variant.10 Jones
et al10 state that keloid BCCs are found in different histological
kinds of BCCs with varying appearances. They found 1.6% of
all BCCs had keloidal collagen in the stroma.10 Misago9 who
reported a case of a keloidal BCC, also found the stroma char-
acteristically demonstrates the prominent keloidal, thickened
collagen bundles and well-circumscribed keloidal collagen
bundles that proliferated in a nodular form. Subsequently, it
has been suggested that keloidal stromal reaction is due to local
inflammatory changes secondary to necrosis or ulceration.10
Furthermore, it has been suggested there may be a correlation
between keloid BCCs and the ear as a site for the development
of keloidal stroma.10,20 However, the tumor described in this
case, in contrast to a keloidal BCC, is rare and to our knowl-
edge has never been reported in the literature. It is unique in
that the common pathological process of a BCC developing
necrosis and ulceration, which in turn cause inflammation and
keloid scar formation, is reversed. In this case, we presented a
keloid scar that has been dormant for 2 years, which improved
under conservative treatment, and then underwent malignant
transformation to a BCC. Since keloid scars can be considered
a tumor, we in fact present a secondary tumor (BCC) which
arises on top of a primary tumor (keloid scar). Furthermore,
He et al13 and Meade et al21 demonstrate another example of
unusual keloid behavior of eruptive keloids associated with
cancer and the clinical importance of giving long-term dynamic
consideration when following a keloid patient.
Figure 4 Rapid regrowth of keloid scar.
Powered by TCPDF (www.tcpdf.org)
OncoTargets and erapy
Publish your work in this journal
Submit your manuscript here: http://www.dovepress.com/oncotargets-and-therapy-journal
OncoTargets and Therapy is an international, peer-reviewed, open
access journal focusing on the pathological basis of all cancers, potential
targets for therapy and treatment protocols employed to improve the
management of cancer patients. The journal also focuses on the impact
of management programs and new therapeutic agents and protocols on
patient perspectives such as quality of life, adherence and satisfaction.
The manuscript management system is completely online and includes
a very quick and fair peer-review system, which is all easy to use. Visit
http://www.dovepress.com/testimonials.php to read real quotes from
published authors.
OncoTargets and Therapy 2016:9
submit your manuscript | www.dovepress.com
Dovepress
Dovepress
Dovepress
4796
Goder et al
Conclusion
Our case study highlights the development of a BBC arising
within a keloid scar to the auricle region after an ear piercing
2 years prior. Keloidal characteristics often occur on the ear;
however, there remain no reports of such a case within the
literature. Given the sparse amount of evidence available,
it is important for clinicians to understand and identify key
keloidal features in BCCs and to reinforce the association of
morphoeiform patterns of growth, ulceration, and necrosis
as described by Jones et al10 Therefore, the authors stress
the importance of considering early biopsy in any rapidly
growing or changing keloidal scar.
Acknowledgment
The authors would like to thank the patient for her
cooperation.
Disclosure
The authors report no conflicts of interest in this work.
References
1. Chung S. Basal cell carcinoma. Arch Plast Surg. 2012;39(2):166–170.
2. Rao J, Deora H. Surgical excision with forehead flap as single modality
treatment for basal cell cancer of central face: single institutional experi-
ence of 50 cases. J Skin Cancer. 2014;2014:1–5.
3. Lim K-R, Cho K-H, Hwang S-M, Jung Y-H, Kim Song J. Basal cell
carcinoma presenting as a hypertrophic scar. Arch Plast Surg. 2013;40(3):
289–291.
4. Sand M, Sand D, Brors D, Altmeyer P, Mann B, Bechara FG. Cutaneous
lesions of the external ear. Head Face Med. 2008;4(2):1–13.
5. Requena L, Martin L, Farina MC, Pique E, Escalonilla P. Keloidal basal
cell carcinoma. A new clinicopathological variant of basal cell carcinoma.
Br J Dermatol. 1996;134(5):953–957.
6. Balestri R, Misciali C, Zampatti C, Odorici G, Balestri JA. Keloidal
basal cell carcinoma: should it be considered a distinct entity? J Dtsch
Dermatol Ges. 2013;11(12):1196–1198.
7. Nagashima K, Demitsu T, Nakamura T, et al. Keloidal basal cell carcinoma
possibly developed from classical nodulo-ulcerative type of basal cell
carcinoma: report of a case. J Dermatol. 2015;42(4):427–429.
8. Misago N, Ogusu Y, Narisawa Y. Keloidal basal cell carcinoma after
radiation therapy. Eur J Dermatol. 2004;14(3):182–185.
9. Misago N. Keloidal basal cell carcinoma. Am J Dermatopathol. 2008;
30(1):87.
10. Jones M, Bresch M, Alvarez D, Böer A. Keloidal basal cell carcinoma:
not a distinctive clinicopathological entity. Br J Dermatol. 2009;160(1):
127–131.
11. Tanaydin V, Beugels J, Piatkowski A, et al. Efficacy of custom-made
pressure clips for ear keloid treatment after surgical excision. J Plast
Reconstr Aesthet Surg. 2016;69(1):115–121.
12. Wilkins RH. Neurosurgical classic. XVII. J Neurosurg. 1964;21:
240–244.
13. He Y, Merin MR, Sharon VR, Maverakis E. Eruptive keloids associated
with breast cancer: a paraneoplastic phenomenon? Acta Derm Venereol.
2011;91(4):480–481.
14. De Sousa RF, Chakravarty B, Sharma A, Parwaz MA, Malik A. Efficacy
of triple therapy in auricular keloids. J Cutan Aesthet Surg. 2014;7(2):
98–102.
15. Del Toro D, Dedhia R, Tollefson TT. Advances in scar management:
prevention and management of hypertrophic scars and keloids. Curr
Opin Otolaryngol Head Neck Surg. 2016; Epub 2016 May 7.
16. Viera MH, Vivas AC, Berman B. Update on keloid management: clinical
and basic science advances. Adv Wound Care. 2012;1(5):200–206.
17. Halim AS, Emami A, Salahshourifar I, Kannan TP. Keloid scarring:
understanding the genetic basis, advances, and prospects. Arch Plast
Surg. 2012;39(3):184–189.
18. Shin JY, Lee JW, Roh SG, Lee NH, Yang KM. A comparison of the
effectiveness of triamcinolone and radiation therapy for ear keloids
after surgical excision: a systematic review and meta-analysis. Plast
Reconstr Surg. 2016;137(6):1718–1725.
19. Park TH, Rah DK. Successful eradication of helical rim keloids with
surgical excision followed by pressure therapy using a combination
of magnets and silicone gel sheeting. Int Wound J. 2015. Epub 2015
November 23.
20. Slemp AE, Kirschner RE. Keloids and scars: a review of keloids and
scars, their pathogenesis, risk factors, and management. Curr Opin
Pediatr. 2006;18(4):396–402.
21. Meade C, Smith S, Makhzoumi Z. Eruptive keloids associated with
aromatase inhibitor therapy. JAAD Case Rep. 2015;1(3):112–113.
Powered by TCPDF (www.tcpdf.org)