Content uploaded by Basem Abbas Ahmed Al-Ubaidi
Author content
All content in this area was uploaded by Basem Abbas Ahmed Al-Ubaidi on Nov 03, 2016
Content may be subject to copyright.
Bahrain Medical Bulletin, Vol. 37, No. 3, September 2015
Education-Family Physician Corner
Acne Keloidalis Nuchae (Folliculitis Keloidalis)
Basem Al Ubaidi, FMAB, MHPE*
Acne Keloidalis Nuchae (AKN) is characterized by multiple follicular-based papules,
pustules, nodules, keloid-like, hypertrophic plaques. AKN typically occurs on the
posterior occipital scalp and develops almost exclusively in young, dark-skinned males.
Early diagnosis of AKN and proper management would have a good outcome, before
progressing to ugly untreatable scarring.
A thirty-five-year-old Indian male presented with slightly itching papules with variable
pain developed from multiple pimples on the posterior occipital region. The patient was
given oral antibiotics (doxycycline) twice daily for four weeks. Thereafter, the patient
was given high-potency topical steroids (0.05% clobetasol propionate) twice a day for
another two weeks. The large keloidal lesions were treated with cryotherapy for three
sessions which resulted in significant lesion regression.
___________________________________________________________________________
* Consultant Family Physician
Ministry of Health
Kingdom of Bahrain
Email: bahmed1@health.gov.bh
Acne (folliculitis) Keloidalis Nuchae (AKN) is recognized as chronic, fibrotic papules,
nodules and pustules which lead to scarring alopecia at the back of the neck and occiput1. It is
usually seen as asymptomatic, keloidal plaques; however, patients may have burning pain or
stubborn pruritus from either pus or multiple oozing sinuses. It would ultimately affect the
patient’s quality of life (QOL) as the scarring is difficult to treat, and it is sometimes seen in
obvious locations2.
The prevalence of AKN is 0.5%; mostly are seen in the dark-skinned individuals of African
descent or black Asian, with a male-to-female frequency rate of 20:1; ages ranges from 14 to
25 years1,3-5.
AKN is either idiopathic or secondary to a direct reaction to hair growth, wearing helmets or
irritation from long, curly/frizzy hair trapped between shirt collars and a fat neck. The
predisposing factors of AKN are constant irritation from foreign body reaction and advanced
fibrosis with low-grade bacterial infections. The physician should be able to differentiate
AKN from other common skin lesions, such as impetigo, acne vulgaris, tinea capitis,
hidradenitis suppurativa, dissecting cellulitis, pseudopélade of Brocq, keloid, and infectious
folliculitis2. The diagnosis of AKN is usually made clinically while a biopsy is necessary
only in atypical cases. In cases that involve the occurrence of abscesses or pustules, it is
necessary to have it drained and sent for culture and sensitivity3,6.
The aim of this presentation is to report a rare case of AKN in a young patient who had
successful outcome after medical treatment.
THE CASE
A thirty-five-year-old Indian male presented with lesions initially manifested as slightly
itching papules with variable pain developed from multiple pimples on the posterior occipital
region. It grew over six months and had become disfiguring, painful and keloid-like plaques.
The patient revealed history of close shaving and chronic rubbing of the area by clothing.
On examination, it was observed that multiple lesions had developed in hair-bearing areas of
the skin. The lesions were firm, dome-shaped, follicular-based papules, pustules and plaques
measuring between 4-5 mm in diameter. Keloid-like papules had merged to form cluster
shape on the posterior of the neck which reached more than 10 cm in diameter. Loss of hair
and damaged hair shafts had been seen within and at boundaries of the plaques with purulent
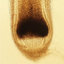
discharge and traumatized lesions when the hair was groomed, see figure 1.
Figure 1: Multiple Papular, Pustular, and Keloid-Like Lesions on the Posterior
Occipital Region
The patient was given oral antibiotics (doxycycline) twice daily for four weeks. Thereafter,
the patient was given high-potency topical steroids (0.05% clobetasol propionate) twice a day
for another two weeks. The large keloidal lesions were treated with cryotherapy for three
sessions which resulted in significant lesion regression.
DISCUSSION
Treatment of AKN is challenging and difficult as the lesions often are intractable. Patients
might present with history of numerous modalities of previous treatment with varying
degrees of success. Early diagnosis and timely treatment of AKN reduces the possibility of
long-term keloidal scarring and disfigurements2.
Our primary goal of treatment was focused on the patient’s education. He was advised to
discontinue wearing possible offending garments that may cause irritation, such as tight
fitting shirts and to instruct his barbers not to shave the posterior part of his hairline. The
patient should avoid hair greases or pomades which could interfere with hair growth. Hair in
the affected area should be kept long to avoid regrowth into the scalp. The patient is advised
to shampoo with gentle foam washes, such as benzoyl peroxide chlorhexidine or mild
keratolytic agents3.
Treatment of AKN is dependent on the lesion type and disease stage; the treatment could be
medical or surgical. The medical could be oral antibiotics and high-potency topical
steroids2,4. Cryotherapy could be used for large keloidal lesions7.
Patients presented with large abscesses, or oozing sinuses should be drained, culture and
sensitivity should be requested and oral antibiotics and oral prednisolone for 7-10 days
duration should be initiated2.
In advanced, intractable AKN, laser ablation (carbon dioxide laser), intralesional
triamcinolone acetonide, 5-fluorouracil or immunotherapy injection (5 to 40 mg/mL) should
be considered8. Surgical excision of the keloidal-scarring plaque includes a horizontal ellipse
with primary closure9,10.
CONCLUSION
AKN is a chronic, folliculitis disease affect mostly adolescent to adult, dark-skinned
males on the nape of the neck or occipital area. An untreated AKN case ultimately
leads to disfigurement, hypertrophic scarring, chronic abscesses and hair loss.
___________________________________________________________________________
Potential Conflicts of interest: None.
Competing interest: None. Sponsorship: None.
Submission date: 21 May 2014. Acceptance date: 22 July 2015.
Ethical Approval: Approved by North Muharraq Health Center, MOH, Bahrain.
REFERENCES
1. Quarles FN, Brody H, Badreshia S, et al. Acne Keloidalis Nuchae. Dermatol Ther
2007; 20(3):128-32.
2. Adegbidi H, Atadokpede F, do Ango-Padonou F, et al. Keloid Acne of the Neck:
Epidemiological Studies over 10 Years. Int J Dermatol 2005; 44 Suppl 1:49-50.
3. Kelly AP. Pseudofolliculitis Barbae and Acne Keloidalis Nuchae. Dermatol Clin
2003; 21(4):645-53.
4. Khumalo NP, Jessop S, Gumedze F, et al. Hairdressing and the Prevalence of Scalp
Disease in African Adults. Br J Dermatol 2007; 157(5):981-8.
5. Kundu RV, Patterson S. Dermatologic Conditions in Skin of Color: Part II. Disorders
Occurring Predominately in Skin of Color. Am Fam Physician 2013; 87(12):859-65.
6. Cole C, Gazewood J. Diagnosis and Treatment of Impetigo. Am Fam Physician 2007;
75(6):859-64.
7. Acne Keloidalis Nuchae. Therapeutic Strategies in Dermatology. Available at:
http://www.derm101.com/therapeutic/acne-keloidalis-nuchae. Accessed on 2.4.2014.
8. Esmat SM, Abdel Hay RM, Abu Zeid OM, et al. The Efficacy of Laser-Assisted Hair
Removal in the Treatment of Acne Keloidalis Nuchae; a Pilot Study. Eur J Dermatol
2012; 22(5):645-50.
9. Bajaj V, Langtry JA. Surgical Excision of Acne Keloidalis Nuchae with Secondary
Intention Healing. Clin Exp Dermatol 2008; 33(1):53-5.
10. Wu WY, Otberg N, McElwee KJ, et al. Diagnosis and Management of Primary
Cicatricial Alopecia: Part II. Skinmed 2008; 7(2):78-83.