Available via license: CC BY-NC 4.0
Content may be subject to copyright.
seen in all cases, until formal histology was obtained,
emphasising the challenges, and need for early appro-
priate specialist input. Whilst the prenatal detection of
craniofacial abnormalities increases, there remain di-
agnostic challenges in differentiating prenatal congeni-
tal midfacial defects in utero. These defects are best
investigated and monitored using prenatal ultrasound
and MRI, to narrow the differential diagnosis, guide
timing of delivery and allow for appropriate surgical
planning. Prenatally detected nasal glioma, may only be
confirmed on histology and families must be counselled
appropriately to prepare them for the possible alterna-
tive diagnoses. Early surgical resection was undertaken
to achieve more favourable aesthetic outcomes, reduce
complications of ocular development and provide de-
finitive histological diagnosis.
© 2014 Baishideng Publishing Group Inc. All rights reserved.
Key words: Nasal glioma; Prenatal; Craniofacial; Imaging
Core tip: Advances in foetal imaging have increased
our detection rate of craniofacial abnormalities in utero.
This enables early surgical input providing differential
diagnosis, surgical planning, timing of delivery and
counselling for families. Seven cases of prenatally diag-
nosed nasal glioma have been reported. The authors
advocate ultrasound and foetal magnetic resonance im-
aging (MRI) to delineate the lesion, exclude intracranial
involvement and monitor size. Foetal MRI also provides
accurate delineation of the upper aerodigestive tract,
allowing clinicians to anticipate airway compromise, in
this otherwise benign condition. Early surgical resection
is advised, for better aesthetic outcomes and to ensure
normal ocular development.
Fox R, Okhovat S, Beegun I. Prenatal diagnosis and management
of nasal glioma. World J Otorhinolaryngol 2014; 4(3): 12-16
Available from: URL: http://www.wjgnet.com/2218-6247/full/
v4/i3/12.htm DOI: http://dx.doi.org/10.5319/wjo.v4.i3.12
Prenatal diagnosis and management of nasal glioma
Richard Fox, Saleh Okhovat, Issa Beegun
Richard Fox, Saleh Okhovat, Issa Beegun, Department of
Otolaryngology, West Middlesex University Hospital, Isleworth,
Middlesex TW7 6AF, United Kingdom
Author contributions: Fox R performed the literature search;
Fox R and Okhovat S screened the cases; Fox R, Okhovat S and
Beegun I reviewed the articles and wrote this paper.
Correspondence to: Dr. Richard Fox, Department of Otolar-
yngology, West Middlesex University Hospital, Twickenham Rd,
Isleworth, Middlesex TW7 6AF,
United Kingdom. richardfox@doctors.org.uk
Telephone: +44-20-85602121
Received: January 18, 2014 Revised: June 10, 2014
Accepted: July 12, 2014
Published online: August 28, 2014
Abstract
Advances in foetal imaging have increased our detec-
tion rate of craniofacial abnormalities in utero. Nasal
glioma is a rare, benign, congenital facial defect. Once
detected, further imaging is required to assess for in-
tracranial communication, the presence of additional
defects, determine the patency of the aerodigestive
tract and decide on timing of delivery. The authors
review the current literature on diagnosis and manage-
ment of nasal glioma in this rapidly advancing field
of craniofacial anomalies detected in utero. Literature
search of EMBASE and MEDLINE databases yielded 594
articles, which were screened by 2 independent review-
ers. A total of 7 papers were selected after exclusion.
There have been seven cases of prenatally diagnosed
nasal glioma. The earliest of these was detected at 20
wk gestation. The majority were investigated with foe-
tal magnetic resonance imaging (MRI) to establish any
intracranial communication or bony defects. Ultrasound
monitoring, doppler waveform and 3D rendered images
were utilised to delineate the lesion, monitor growth
and differentiate potential diagnosis. Postnatal MRI is
favoured by most to re-evaluate the lesion and aid sur-
gical planning. Surgical resection was performed within
the first few months of life. Diagnostic uncertainty was
MINIREVIEWS
12 August 28, 2014
|
Volume 4
|
Issue 3
|
WJO
|
www.wjgnet.com
World Journal of
Otorhinolaryngology
W J O
Submit a Manuscript: http://www.wjgnet.com/esps/
Help Desk: http://www.wjgnet.com/esps/helpdesk.aspx
DOI: 10.5319/wjo.v4.i3.12
World J Otorhinolaryngol 2014 August 28; 4(3): 12-16
ISSN 2218-6247 (online)
© 2014 Baishideng Publishing Group Inc. All rights reserved.
INTRODUCTION
Advances in foetal imaging have improved our detec-
tion rate of craniofacial abnormalities in utero. These
improvements allow for earlier diagnosis, which can be
made as early as the 11th week of gestation[1]. As such, the
Head and neck surgeon is thrust into a new role in foetal
management as part of the multidisciplinary team, pro-
viding differential diagnosis, advising on timing of birth
and postnatal surgical planning.
While craniofacial abnormalities are uncommon, the
most frequently occurring include; encephaloceles, nasal
gliomas and nasal dermal sinus cysts. The differential
detectable on prenatal ultrasound also includes haeman-
giomas, dacryocystocele, teratoma and retinoblastoma[2].
These pathologies are of interest to maxillofacial, head
and neck, ophthalmology and neurosurgeons alike and
their role is integral in the psychosocial counselling of the
parents, preparing them for delivery and discussion of
treatment options and their timing. The authors’ review
the reported cases of prenatal diagnosis and management
of nasal glioma and review the literature on this rapidly
advancing field of craniofacial anomalies detected in
utero.
NASAL GLIOMA
Nasal Glioma is a rare, benign, congenital facial lesion
occurring in 1:20000-40000 live births[3]. They are com-
prised of heterotopic neuroglial tissue, arising in the mid-
line and are most commonly extranasal (60%)[4] (Figure
1) but may be intranasal (30%) or display both extra and
intranasal components (10%)[2]. It is important to dif-
ferentiate nasal glioma from an anterior encephalocele,
which involves a herniation of meninges through an
incompletely closed fontanel, retaining intracranial com-
munication, requiring neurosurgical assessment[5].
Prenatal ultrasound is typically used to conrm ges-
tational age, foetal number, monitor foetal well being
and detect gross abnormalities[6]. Modern ultrasound
technology provides accurate multiplanar views of the
foetal face via surface rendered images of 3D ultrasound,
maintaining its prominent role in antenatal care[7,8]. Such
advances have increased the detection rate of craniofacial
abnormalities that once would not have been appreciated.
Complications of nasal glioma depend on its location
and include nasal deformity, amblyopia, impaired visual
eld and nasal obstruction. As neonates are obligate nasal
breathers this poses a threat to the foetal airway, requiring
accurate delineation of the lesion and involvement of the
appropriate specialists within the multidisciplinary team
(MDT) that can address parental questions and anxiety
and facilitate pre and postnatal planning.
Foetal magnetic resonance imaging (MRI) is favoured
by most, to provide more accurate soft tissue imaging,
confirm equivocal findings and identify intracranial in-
volvement in utero[9]. It avoids unnecessary irradiation
of mother and foetus and is favoured over computed
tomography (CT). Is also provides synchronous iden-
tification of abnormalities of the upper aerodigestive
tract, delineation of the foetal airway and ensures a well
rehearsed MDT is prepared for denitive intra or post-
partum airway interventions, should they be required[10].
Foetal MRI is not however considered an appropriate
alternative to ultrasound, which can also provide doppler
characteristics, and MRI should not be performed in iso-
lation for foetal screening[6].
Should foetal MRI raise concerns of foetal airway
compromise, intrapartum procedures can be performed
to treat predicted complications of postpartum airway
obstruction. The Ex-Utero Intrapartum Procedure uti-
lises the utero-placental circulation, providing foetal
oxygenation for up to 30-60 min[11]. Life saving airway in-
terventions can be made on the partially delivered foetus
whilst the mother is under general anaethesia. Manage-
ment using this procedure requires detailed planning and
a highly specialised, well-rehearsed MDT[11].
SEARCH CRITERIA
The literature search was conducted on two electronic
databases, MEDLINE and EMBASE with titles includ-
ing “Glioma”, “Prenatal”, “In Utero” and “Craniofacial”
published from 1980 to present. Two independent re-
viewers screened 594 articles, and articles with repeti-
tion/duplication of original data, animal studies and
studies written in non-english language were exclude. We
were guided by the PRISMA checklist and ow diagram
for article selection (Figure 2). A total of 7 papers were
selected.
To date, very little has been published on prenatal
management of nasal gliomas. There are seven cases re-
porting prenatally detected nasal glioma in the literature,
summarised in Table 1. Five of these were successfully
managed with good outcomes, one lead to termination
of pregnancy and one resulted in death secondary to
post-operative neonatal infection.
CASE REVIEW
Chmait et al[12] (2002) were the rst to report a prenatal
diagnosis of nasal glioma in the literature. At 31 wk of
13 August 28, 2014
|
Volume 4
|
Issue 3
|
WJO
|
www.wjgnet.com
Fox R
et al
. Prenatal nasal glioma review
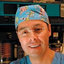
Figure 1 Clinical image of Nasal glioma in a neonate (original image with
permission)[13].
gestation they identied a 19 mm × 15 mm left paraor-
bital cystic mass on 2D ultrasound scan. 3D ultrasound
was performed and generated a surface rendered image
of the foetal face, leading to a preliminary diagnosis of a
dacryocystocele. No Doppler ow was present within the
mass and no further prenatal imaging was undertaken.
The baby was delivered at term via uncomplicated
spontaneous vaginal delivery, with a 20 mm rm, extra-
nasal lesion in the left nasoglabellar region. The diagnosis
was still inconclusive and postnatal MRI was performed,
showing a distinct mass with no intercranial communica-
tion. The lesion was excised at 3 mo of age, using a fore-
head ap, and histological analysis conrmed a diagnosis
of nasal glioma.
Beegun et al[13] (2012) reported the earliest prenatal
detection of nasal glioma, at 20 wk gestation. A 10 mm
× 10 mm × 9 mm left paraorbital soft tissue mass was
reported on repeat ultrasound scan at 23 wk gestation.
It demonstrated a single vessel supply but its origin and
communication with the foetal brain could not be deter-
mined. Foetal MRI and repeat ultrasound were undertak-
en at 24 wk and showed the lesion had grown to 13 mm
× 11 mm × 12 mm. The foetal brain appeared normal
and was not in communication with the lesion. Repeat
ultrasound scans were performed every two weeks to
monitor the lesions size, which remained stable until 28
wk, where it increased to 16 mm × 12 mm. Repeat MRI
at 28 wk and 36 wk did not show any associated bony
erosion or deep extension. At this time the diagnosis was
still in question.
The baby was delivered at 38 wk via uncomplicated
spontaneous vaginal delivery, with a 20 mm × 15 mm
soft cystic mass in the left nasoglabellar region, suspected
to be a haemangioma. The lesion grew to 30 mm × 40
mm by 2 mo of age. A postnatal MRI excluded bony
involvement however there were concerns that the le-
sion may obstruct the baby’s binocular vision and surgical
excision with primary closure was undertaken at 2 mo of
age and histology conrmed a diagnosis of nasal glioma.
Both De Biasio et al[2] (2006) and Grzegorczyk et al[9]
(2010) report prenatal diagnosis of nasal glioma at 22 wk
gestation. Basio detected a 7 mm lesion, with no doppler
blood flow and undertook a foetal MRI that excluded
intracranial communication and bone involvement, but
no specific diagnosis could be made. Ultrasound moni-
toring showed the lesion increased in size to 20 mm at 32
wk gestation. The baby was delivered at 38 wk gestation
via uncomplicated spontaneous vaginal delivery, with a
20 mm pink non-compressible mass medial to the left
internal canthus. Postnatal MRI suggested a diagnosis of
nasal glioma with partial intranasal extension. The lesion
was excised at 4 mo of age and histology conrmed the
diagnosis. Similarly, Grzegorczyk et al[9] identied a vascu-
lar hypoechoic mass on the left nasal bone on ultrasound
scan. This was also investigated with foetal MRI that
excluded intracranial communication and bony erosion.
Following delivery, the lesion appeared as a reddish mass,
suspected to be a haemangioma. Postnatal imaging fur-
ther established low velocity ow consistent with a nasal
glioma that was removed at 5 mo of age and the diagno-
sis was conrmed with histology.
Okumura et al[14] (2012) described a recent case of a
craniofacial anomolie detected in the third trimester. A fa-
cial mass protruding from the left nostril with no doppler
ow was identied at 33 wk gestation. No additional pre-
natal imaging was undertaken and the baby was delivered
at 35 wk gestation via spontaneous vaginal delivery and
immediately intubated. Postnatal CT scan was undertaken
on day 8, and suggested an osseous defect the ethmoid
bone with herniation of intracranial contents into the
nasal cavity. A preliminary diagnosis of transethmoidal
encephalocele was made. This was revised following
postnatal MRI that demonstrated no intracranial involve-
ment or bony defect, utilising better soft tissue delinea-
tion. An intranasal glioma was suspected and excised via
endoscopic intranasal and oral routes, and the diagnosis
was conrmed on histology. This case was complicated
by the development of a lower respiratory tract infection
and subsequent neonatal death.
Ajose-Popoola et al[5] (2011) described the manage-
ment of a nasal glioma in a 3 mo old child, who had a
25 mm × 25 mm non-pulsatile solid nasoglabellar mass
detected on prenatal ultrasound. It was subsequently
investigated with foetal MRI that showed the mass was
separated from brain parenchymal by a distinct cerebro-
spinal uid plane. The baby was delivered without com-
plication and postnatal MRI revealed a 28 mm × 18 mm
× 18 mm mass in the midline, with possible intracranial
communication through an anterior bony defect. Postna-
tal CT was undertaken at 3 mo of age, and showed the
lesion had grown to a 28 mm × 20 mm × 20 mm mass
that appeared to have intracranial connection via a 8 mm
× 6 mm bony defect of the glabella and metopic suture.
The lesion was excised via a midline nasal incision and no
communication with the intracranial vault was seen. His-
tology conrmed a diagnosis of nasal glioma.
Tonni et al[4] (2011) described a second trimester de-
tection of a midline craniofacial anomolie. Further ex-
14 August 28, 2014
|
Volume 4
|
Issue 3
|
WJO
|
www.wjgnet.com
Initial search of EMBASE and
MEDLINE databases’ yielded
594 papers
Two independent reviewers
reviewed all the titles
identified (
n
= 594)
Full text articles assessed
for eligibility (
n
= 18)
Included papers for
final review (
n
= 7)
Excluded records
(
n
= 576)
Full-text articles excluded,
non-english language, failed
to comment on prenatal
diagnosis (
n
= 11)
Figure 2 PRISMA ow diagram for inclusion/exclusion.
Fox R
et al
. Prenatal nasal glioma review
amination via amniocentesis showed a 46,xx Karyotype
with elevated α-FP levels. The parents declined further
antenatal investigation and opted for legal termination of
pregnancy in view of the severe psychophysical distur-
bances associated with the detection of the abnormality
with life threatening risks to the mother. Tissue obtained
by necropsy conrmed the diagnosis of nasal glioma.
DISCUSSION
Nasal glioma is a rare benign congenital midline facial de-
fect that is being detected in the prenatal period with in-
creasing frequency[2]. Advances in foetal imaging provide
more accurate delineation of the foetal face. Ultrasound
scanning is still the dominant antenatal imaging modality
in modern obstetrics. The use of 3D rendered images
along with doppler waveforms show characteristics that
allows specialists to narrow their differential diagnosis[12].
An anterior encephalocele, appears as a midline cystic
or solid mass emanating from a calvarial defect and may
be accompanied by ventriculomegaly[2]. Haemangioma
demonstrates a typical doppler blood ow pattern, high
during arterial diastole, within a septate or solid mass
protruding from the skull[2]. Nasal glioma are firm and
nonpulsatile masses, most commonly originating from
the nasoglabellar region, with low ow on doppler signal.
Retinoblastoma appear as a heterogeneous mass arising
directly from the orbit, with an irregular echogenic struc-
ture and covering membrane[2].
Beegun et al[13] emphasised the value of ultrasound in
monitoring lesion size, using two-weekly ultrasound with
repeated prenatal MRI to exclude bony erosion associ-
ated with lesion growth, in order to guide prenatal plans
and timing of birth (Figure 3). Chmait et al[12], supports
the use of 3D rendered ultrasound images but under-
scored the difculty in achieving an accurate prenatal di-
agnosis. These cases all shared diagnostic uncertainty and
each had an alternative working diagnosis, with diagnostic
conrmation only being conrmed as nasal glioma with
histological analysis.
Antenatal MRI is the modality of choice to investigate
craniofacial abnormalities in utero and was performed
in all except two cases; one was declined by parents who
opted for termination of pregnancy, the other when the
anomaly was detected late, in the third trimester. T1-
weighted MRI demonstrates nasal glioma to be isointense
to grey matter, with moderate contrast enhancement[4].
T2 weighted imaging will show hypointense mass similar
to a congenital haemangioma, with low resistance arterial
ow on doppler imaging[4]. It is important to identify any
intracranial communication and exclude the presence of
an anterior encephalocele. This distinction was unclear in
two cases where a suggestion of intracranial communica-
tion was present even after postnatal imaging. Okumura
et al[14] opted for initial postnatal CT to delineate the le-
sion. This suggested a small anterior calvarial bony de-
fect; leading to a preliminary diagnosis of transethmoidal
encephalocele that was revised once postnatal MRI was
repeated. This emphasises the diagnostic difficulties in-
herent with these lesions. MRI is generally favoured over
CT as it is at least as accurate as CT in detecting intracra-
nial extension and avoids radiation to the head, neck and
radiosensitive lens[15].
Grzegorczyk et al[9] recommends that pre and postna-
tal MRI should be performed, where available, in all cases
where a craniofacial defect is detected on ultrasound.
This can exclude intracranial extension, identify addi-
tional abnormalities, allow accurate planning of surgical
15 August 28, 2014
|
Volume 4
|
Issue 3
|
WJO
|
www.wjgnet.com
Table 1 Summarising the management of prenatal nasal glioma
Ref. Gestational age at detection Prenatal Ix Postnatal Ix Age at surgery Outcome
Chmait et al[12], 2002 31 wk Ultrasound + 3D image MRI 3 mo Complete excision-forehead
ap
Di Biasio et al[2], 2006 22 wk Ultrasound (inc. Doppler) and MRI MRI 4 mo Complete excision
Grzegorczyk et al[9], 2010 22 wk Ultrasound (inc. Doppler) and MRI MRI 5 mo Complete excision
Ajose-Popoola et al[5], 2011 Second trimester Ultrasound (inc. Doppler) and MRI CT and MRI 3 mo Complete excision
Tonni et al[4], 2011 Second trimester Ultrasound (inc. Doppler) and
Amniocentesis
N/A N/A Termination of pregnancy:
elevated α-FP
Okumura et al[14], 2012 33 wk Ultrasound (inc. Doppler) CT and MRI 8 d Nasal and extranasal
excision
Neonatal death
secondary to LRTI
Beegun et al[13], 2012 20 wk Ultrasound (inc. Doppler) and MRI MRI 2 mo Complete excision
MRI: Magnetic resonance imaging; CT: Computed tomography; N/A: Not applicable.
Figure 3 Sagittal foetal magnetic resonance imaging in utero, identifying
nasal lesion (arrow). Original image with permission[13].
Fox R
et al
. Prenatal nasal glioma review
approach, and reduce risks of incomplete resection.
CONCLUSION
Prenatal diagnosis of nasal glioma may be suggested as
early as the second trimester, but diagnostic certainty is
rarely achievable until postnatal imaging or histological
examination. Investigations may suggest or exclude cer-
tain diagnosis but families must be counselled accordingly
to ensure they are fully prepared for all possible diagnos-
tic eventualities.
Doppler ultrasound provides important detection and
monitoring facilities to guide pre and postnatal planning
and direct the working diagnosis, differentiating glioma
from haemangioma.
Prenatal MRI improves the diagnostic accuracy of
ultrasound but should not be employed as an indepen-
dent screening tool. Foetal MRI can identify associated
intracranial communication, additional lesions, cerebral
defects and delineate the upper aerodigestive tract of the
neonate, predicting airway complications and allowing
appropriate planning. Postnatal MRI imaging is essential
to accurately identify the lesion, and is as good if not
superior to CT in identifying intracranial extension, with
the added benet of avoiding neonatal exposure to ionis-
ing radiation[15]. It is also important to identify the glioma
stalk, as full excision is required to reduce risk of recur-
rence, cerebrospinal uid leak and meningitis.
When radiological investigations are combined with
chorionic villous and or amniocentesis, the clinicians are
provided with valuable diagnostic and prognostic infor-
mation that may be used to empower families and inform
a multidisciplinary discussion regarding genetic counsel-
ling, timing of delivery, postnatal treatment options and
surgical planning[13]. The importance of this aspect of
prenatal care cannot be underestimated, as the psychoso-
cial impact of detecting these prenatal anomalies can be
great.
Early surgical intervention is recommended, and is
believed to correlate with more favourable aesthetic out-
comes, reduce complications of ocular development and
provide denitive histological diagnosis. Once a diagnosis
of nasal glioma is confirmed, the overall prognosis is
favourable, with low recurrence rate following complete
excision.
REFERENCES
1 Ettema AM, Wenghoefer M, Hansmann M, Carels CE,
Borstlap WA, Bergé SJ. Prenatal diagnosis of craniomaxil-
lofacial malformations: a characterization of phenotypes in
trisomies 13, 18, and 21 by ultrasound and pathology. Cleft
Palate Craniofac J 2010; 47: 189-196 [PMID: 19860526 DOI:
10.1597/08-285.1]
2 De Biasio P, Scarso E, Prefumo F, Odella C, Rossi A, Ven-
turini PL. Prenatal diagnosis of a nasal glioma in the mid
trimester. Ultrasound Obstet Gynecol 2006; 27: 571-573 [PMID:
16570265 DOI: 10.1002/uog.2754]
3 Strauss RB, Callicott JH, Hargett IR. Intranasal neuroglial
heterotopia. So-called nasal glioma. Am J Dis Child 1966; 111:
317-320 [PMID: 4159440 DOI: 10.1001/archpedi.1966.02090060
127019]
4 Tonni G, Lituania M, Bonasoni MP, De Felice C. Prenatal
ultrasound and histological diagnosis of fetal nasal glioma
(heterotopic central nervous system tissue): report of a new
case and review of the literature. Arch Gynecol Obstet 2011;
283 Suppl 1: 55-59 [PMID: 21331541 DOI: 10.1007/s00404-01
1-1856-3]
5 Ajose-Popoola O, Lin HW, Silvera VM, Teot LA, Madsen JR,
Meara JG, Rahbar R. Nasal glioma: prenatal diagnosis and
multidisciplinary surgical approach. Skull Base Rep 2011; 1:
83-88 [PMID: 23984207 DOI: 10.1055/s-0031-1284210]
6 Robson CD, Barnewolt CE. MR imaging of fetal head and
neck anomalies. Neuroimaging Clin N Am 2004; 14: 273-291,
viii [PMID: 15182819 DOI: 10.1016/j.nic.2004.03.005]
7 Costello BJ, Edwards SP. Prenatal diagnosis and treatment
of craniomaxillofacial anomalies. Oral Maxillofac Surg Clin
North Am 2010; 22: 5-15 [PMID: 20159474 DOI: 10.1016/j.
coms.2009.10.003]
8 Pretorius DH, Nelson TR. Fetal face visualization using
three-dimensional ultrasonography. J Ultrasound Med 1995;
14: 349-356 [PMID: 7609012]
9 Grzegorczyk V, Brasseur-Daudruy M, Labadie G, Cellier
C, Verspyck E. Prenatal diagnosis of a nasal glioma. Pediatr
Radiol 2010; 40: 1706-1709 [PMID: 20401478 DOI: 10.1007/s00
247-010-1642-6]
10 Husein OF, Collins M, Kang DR. Neuroglial heterotopia
causing neonatal airway obstruction: presentation, manage-
ment, and literature review. Eur J Pediatr 2008; 167: 1351-1355
[PMID: 18758813 DOI: 10.1007/s00431-008-0810-2]
11 Taghavi K, Beasley S. The ex utero intrapartum treatment
(EXIT) procedure: application of a new therapeutic para-
digm. J Paediatr Child Health 2013; 49: E420-E427 [PMID:
23662685 DOI: 10.1111/jpc.12223]
12 Chmait RH, Pretorius DH, Hull AD. Nasal glioma. Ultra-
sound Obstet Gynecol 2002; 20: 417-418 [PMID: 12383332 DOI:
10.1046/j.1469-0705.2002.00811.x]
13 Beegun I, Dua R, Connor S, Bentley R. Prenatal diagnosis
and management of a craniofacial glioma detected at 20
weeks’ gestation. Case report and review of the literature.
Int J Oral Maxillofac Surg 2012; 41: 200-202 [PMID: 22137638
DOI: 10.1016/j.ijom.2011.11.003]
14 Okumura M, Francisco RP, Lucato LT, Zerbini MC, Zugaib
M. Prenatal detection and postnatal management of an in-
tranasal glioma. J Pediatr Surg 2012; 47: 1951-1954 [PMID:
23084215 DOI: 10.1016/j.jpedsurg.2012.06.008]
15 Huisman TA, Schneider JF, Kellenberger CJ, Martin-Fiori E,
Willi UV, Holzmann D. Developmental nasal midline masses
in children: neuroradiological evaluation. Eur Radiol 2004; 14:
243-249 [PMID: 12904880 DOI: 10.1007/s00330-003-2008-3]
P- Reviewer: Baglaj SM, Freiherr J, Rossi AC
S- Editor: Wen LL L- Editor: A E- Editor: Liu SQ
16 August 28, 2014
|
Volume 4
|
Issue 3
|
WJO
|
www.wjgnet.com
Fox R
et al
. Prenatal nasal glioma review
© 2014 Baishideng Publishing Group Inc. All rights reserved.
Published by Baishideng Publishing Group Inc
8226 Regency Drive, Pleasanton, CA 94588, USA
Telephone: +1-925-223-8242
Fax: +1-925-223-8243
E-mail: bpgofce@wjgnet.com
Help Desk: http://www.wjgnet.com/esps/helpdesk.aspx
http://www.wjgnet.com