Content uploaded by Takashi Shiihara
Author content
All content in this area was uploaded by Takashi Shiihara on Aug 04, 2015
Content may be subject to copyright.
11. Di Rocco F, Caldarelli M, Di Rocco C: Extrapontine myelinolysis in a
child operated on for a craniopharyngioma. Pediatr Neurosurg
2001;34:166–167.
12. McComb RD, Pfeiffer RF, Casey JH, et al: Lateral pontine and extrapon-
tine myelinolysis associated with hypernatremia and hyperglycemia.
Clin Neuropathol 1989;8:284–288.
13. Finlayson MH, Snider S, Oliva LA, Gault MH: Cerebral and pontine
myelinolysis.
J Neurol Sci 1973;18:399–409.
14. Lebovitz HE: Diabetic ketoacidosis.
Lancet 1995;345:767–772.
15. Glaser N, Barnett P, McCaslin I, et al: Risk factors for cerebral edema
in children with diabetic ketoacidosis.
N Engl J Med 2001;344:264–269.
16. Brown WD: Osmotic demyelination disorders: Central pontine and
extrapontine myelinolysis.
Curr Opin Neurol 2000;13:691–697.
17. Lee JM, Zipfel GJ, Choi DW: The changing landscape of ischaemic brain
injury mechanisms.
Nature 1999;399(Suppl):A7–14.
18. Hynson JL, Kornberg AJ, Coleman LT, et al: Clinical and neuroradio-
logic features of acute disseminated encephalomyelitis in children.
Neu-
rology 2001;56:1308–1312.
Microcephaly, Cerebellar Atrophy, and Focal
Segmental Glomerulosclerosis in Two Brothers: A
Possible Mild Form of Galloway-Mowat Syndrome
ABSTRACT
We report two brothers with microcephaly, cerebellar atrophy,
and focal segmental glomerulosclerosis. The elder brother showed
nephrotic syndrome from 2 years of age and died of renal failure
at 8 years of age. The younger brother showed mild proteinuria from
2 years of age, and his renal function was still preserved at 15 years
of age. We propose that our patients may be affected with a mild
form of Galloway-Mowat syndrome or another autosomal reces-
sive syndrome with focal segmental glomerulosclerosis and cen-
tral nervous system abnormalities. (J Child Neurol 2003;18:147–149).
In 1968, Galloway and Mowat described two siblings with early-
onset nephrotic syndrome, congenital microcephaly, and hiatal
hernias.
1
Since then, more than 30 additional cases with the asso-
ciation of nephrotic syndrome and microcephaly or brain malfor-
mations have been reported as Galloway-Mowat syndrome or
related disorders.
1–16
Familial cases suggest that Galloway-Mowat
syndrome is an autosomal recessive disorder. Nephrotic syndrome
usually manifests within the first 3 years of life and is refractory
to treatment. Most patients die of renal failure before the age of 6
years, although renal histologic findings are not uniform. The cen-
tral nervous system abnormalities are also diverse, such as micro-
cephaly, polymicrogyria, pachygyria, white-matter abnormality,
and cerebellar atrophy. We describe two brothers with micro-
cephaly, cerebellar atrophy, and focal segmental glomerulosclerosis.
We propose a possible mild case of Galloway-Mowat syndrome or
another autosomal recessive syndrome with focal segmental
glomerulosclerosis and central nervous system abnormalities.
Case Reports
Patient 1
A male infant, the first child of healthy, nonconsanguineous parents, was
born at 43 weeks of gestation by vacuum delivery without complication. His
birthweight was 3030 g (
20.4 SD), length was 50.0 cm (+0.2 SD), and head
circumference was 33.0 cm (+0.4 SD). Although he developed normally dur-
ing infancy (ie, smiling at 2 months of age, head control at 3 months, sit-
ting unsupported at 7 months), he subsequently revealed growth delay and
psychomotor retardation. He began to speak at 18 months but was unable
to walk throughout his life.
At 3 years and 9 months of age, he was referred to us for evaluation
of proteinuria. His height was 74 cm (
26.8 SD), weight was 12.0 kg (21.7 SD),
and head circumference was 45.5 cm (
22.7 SD). Physical examination
revealed a high arched palate and no edema. Neurologic examination
revealed mental retardation, accelerated deep tendon reflex, extensor
planter reflex, ankle clonus, muscle hypotonia, and dysmetria. The results
of laboratory examinations were as follows: white blood cell 14.0
3 10
3
/µL,
hemoglobin 14.0 g/dL, total protein 5.0 g/dL, blood urea nitrogen 14 mg/dL,
serum creatinine level 0.5 mg/dL, total cholesterol 341 mg/dL, C3 83 mg/dL,
C4 34 mg/dL, CH50 40.1 CH50 U/mL, proteinuria 1.5 g/day, and no hematuria.
Brain computed tomography demonstrated cerebellar atrophy. Light
microscopy of the renal biopsy specimen showed a segmental increase in
mesangial cellularity and matrix, and immunofluorescence microscopy
revealed deposits of IgM and C3.
His nephrotic syndrome was refractory to treatment with prednisolone,
cyclophosphamide, heparin, and dipyridamole. His renal function gradually
deteriorated, and peritoneal dialysis was introduced at 8 years of age. How-
ever, he died of renal failure soon after. Postmortem examination was not
permitted.
Brief Communications 147
Figure 1. Facial appearance of patient 2. Note narrow forehead,
micrognathia, and esotropia.
Patient 2
A male infant, the third child of the same parents as patient 1, was born at
40 weeks of gestation by spontaneous delivery with no complications.
Birthweight was 3420 g (+0.5 SD), length was 50.5 cm (+0.5 SD), and head
circumference was 35.0 cm (+1.0 SD). His psychomotor development dur-
ing infancy was as follows: smiling at 1 month of age, head control at 3
months, rolling at 6 months, and sitting unsupported at 12 months. At 2 years
of age, he was still unable to speak or walk, and proteinuria was detected.
Muscular biopsy revealed type 1 fiber predominance and a decrease in the
activity of cytochrome
c oxidase.
At 15 years of age, his height was 164 cm (
20.6 SD), weight was 30
kg (
22.8 SD), and head circumference was 50.5 cm (23.5 SD). Physical exam-
ination revealed a narrow forehead, high arched palate, micrognathia,
scoliosis, and arachnodactyly (Figure 1). Neurologic examination revealed
bilateral abducens palsy, alternating esotropia, accelerated deep tendon
reflex, extensor plantar reflex, ankle clonus, muscle hypotonia, dysmetria,
and severe mental retardation. The results of laboratory examination were
as follows: total protein 6.6 g/dL, albumin 3.5 g/dL, blood urea nitrogen 11
mg/dL, serum creatinine level 0.3 mg/dL, IgG 1300 mg/dL, IgA 249 mg/dL,
IgM 174 mg/dL, C3 68 mg/dL, C4 18 mg/dL, CH50 39.3 CH50/mL, creatinine
clearance ratio 143.7 mL/min, and proteinuria 3.2 g/day. Other laboratory
examinations were performed with normal results, including complete
blood cell counts, serum electrolytes, blood gases, blood lactate, blood pyru-
vate, serum and urinary amino acids, activity of leukocyte lysosomal
enzymes, very-long-chain fatty acids in plasma, transferrin electrophore-
sis, chromosomal analysis, mitochondrial DNA analysis (whole mito-
chondrial DNA sequences were determined), and urinary organic acids. The
148 Journal of Child Neurology / Volume 18, Number 2, February 2003
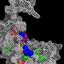
Figure 2. T
2
-weighted (TR 3540 ms, TE 96 ms) images of patient 2 at
16 years of age. A, Axial view at the level of basal ganglia. Cerebral
white matter shows diffusely poor myelination. Cerebral cortex and
deep nuclei are normal. B, Axial view at the level of lower midbrain.
Bilateral cerebellar hemispheres are atrophic or hypoplastic, whereas
the left hemisphere is compressed by a subarachnoidal cyst. C, Mid-
sagittal view. Cerebellar vermis shows atrophy or hypoplasia. Corpus
callosum is deformed.
A
C
B
examination of cerebrospinal fluids, including cell count, protein, glu-
cose, lactate, and pyruvate, was also normal. Brain magnetic resonance
imaging showed poor myelination of the cerebral white matter and diffuse
cerebellar atrophy (Figure 2). Skeletal radiography showed no abnor-
mality except scoliosis. Renal sonography showed no abnormality. Elec-
trophysiologic studies including electroencephalography, brainstem auditory
evoked potentials, and nerve conducting velocities were normal. Light
microscopy of the renal biopsy specimen showed focal segmental hyali-
nosis and sclerosis, and immunofluorescence studies were negative for
all immunoglobulins and complements. Electron microscopy revealed
that the foot process of podocytes was extensively effaced. The mesangial
matrix was expanding, but there was neither cellular proliferation nor
electron-dense deposits present.
Discussion
The Galloway-Mowat syndrome involves both kidney and brain,
although their pathologic findings are heterogeneous.
1–16
The
glomerular findings by light microscopy have been previously
described as normal, mesangial proliferation, focal segmental
glomerulosclerosis, or microcystic dysplasia. The major abnor-
mality found by electron microscopy is the variable thickness of
the glomerular basement membranes. Foot processes and
endothelial cells were also affected. The central nervous system
abnormalities in Galloway-Mowat syndrome are also
diverse.
3,4–7,9,11–13,15
Microcephaly is a major element of Galloway-
Mowat syndrome and is associated with other central nervous sys-
tem abnormalities, consisting of migrational anomalies (ie,
polymicrogyria, agyria, pachygyria), hypomyelination, and cere-
bellar atrophy. Meyers et al proposed that there may be at least
three separate syndromes associated with nephrotic syndrome,
microcephaly, and developmental delay: Galloway-Mowat syn-
drome, a second syndrome of microcephaly, nephrotic syndrome
and developmental delay, and a third syndrome of microcephaly,
nephrotic syndrome, and developmental delay with skeletal dys-
plasia.
17
In the latter two syndromes, the onset of the nephrotic
syndrome is later than that in Galloway-Mowat syndrome (usu-
ally over 3 years), and central nervous system abnormalities
other than microcephaly were not reported. Renal manifesta-
tion in our patients was milder than those of previously reported
cases of Galloway-Mowat syndrome, and central nervous system
abnormalities other than microcephaly did not fit the findings of
a syndrome of microcephaly, nephrotic syndrome, and develop-
mental delay. Our patients could have a mild form of Galloway-
Mowat syndrome or another autosomal recessive syndrome with
focal segmental glomerulosclerosis and central nervous system
abnormalities.
Takashi Shiihara, MD
Mitsuhiro Kato, MD, PhD
Toshiyuki Kimura, MD, PhD
Akira Matsunaga, MD, PhD
Department of Pediatrics
Yamagata University School of Medicine
Yamagata, Japan
Kensuke Joh, MD, PhD
Division of Clinical Investigation
Sakura National Hospital
Chiba, Japan
Kiyoshi Hayasaka, MD, PhD
Department of Pediatrics
Yamagata University School of Medicine
Yamagata, Japan
Received Sept 23, 2002. Received revised Nov 15, 2002. Accepted for pub-
lication Nov 15, 2002.
Address correspondence to Dr Takashi Shiihara, Department of Pediatrics,
Yamagata University School of Medicine, 2-2-2 Iida-nishi, Yamagata, 990-
9585, Japan. Tel: +81-23-628-5329; fax: +81-23-628-5332; e-mail:
shiihara@med.id.yamagata-u.ac.jp.
References
1. Galloway WH, Mowat AP: Congenital microcephaly with hiatus her-
nia and nephrotic syndrome in two sibs. J Med Genet 1968;5:319–321.
2. Shapiro LR, Duncan PA, Farnsworth PB, Lefkowitz M: Congenital
microcephaly, hiatus hernia and nephrotic syndrome: An autosomal
recessive syndrome.
Birth Defects Orig Artic Ser 1976;12:275–278
3. Robain O, Deonna T: Pachygyria and congenital nephrosis disorder
of migration and neuronal orientation.
Acta Neuropathol (Berl)
1983;60:137–141.
4. Palm L, Hagerstrand I, Kristoffersson U, et al: Nephrosis and distur-
bances of neuronal migration in male siblings—A new hereditary dis-
order?
Arch Dis Child 1986;61:545–548.
5. Roos RA, Maaswinkel Mooy PD, vd Loo EM, Kanhai HH: Congenital
microcephaly, infantile spasms, psychomotor retardation, and nephrotic
syndrome in two sibs.
Eur J Pediatr 1987;146:532–536.
6. Kozlowski PB, Sher JH, Nicastri AD, Rudelli RD: Brain morphology
in the Galloway syndrome.
Clin Neuropathol 1989;8:85–91.
7. Cooperstone BG, Friedman A, Kaplan BS: Galloway-Mowat syndrome
of abnormal gyral patterns and glomerulopathy.
Am J Med Genet
1993;47:250–254.
8. Cohen AH, Turner MC: Kidney in Galloway-Mowat syndrome: Clini-
cal spectrum with description of pathology.
Kidney Int
1994;45:1407–1415.
9. Garty BZ, Eisenstein B, Sandbank J, et al: Microcephaly and congen-
ital nephrotic syndrome owing to diffuse mesangial sclerosis: An
autosomal recessive syndrome.
J Med Genet 1994;31:121–125.
10. Yu CH, Tsai WS, Wang PJ, et al: Congenital nephrotic syndrome with
microcephaly: Report of a case.
J Formos Med Assoc 1994;93:528–530.
11. Hou JW, Wang TR: Galloway-Mowat syndrome in Taiwan.
Am J Med
Genet 1995;58:245–248.
12. Kingo AR, Battin M, Solimano A, et al: Further case of Galloway-
Mowat syndrome of abnormal gyral patterns and glomerulopathy.
Am J Med Genet 1997;69:431.
13. Kucharczuk K, de Giorgi AM, Golden J, et al: Additional findings in Gal-
loway-Mowat syndrome.
Pediatr Nephrol 2000;14:406–409.
14. de Vries BB, van’tHoff WG, Surtees RA, Winter RM: Diagnostic dilem-
mas in four infants with nephrotic syndrome, microcephaly and severe
developmental delay.
Clin Dysmorphol 2001;10:115–121.
15. Lin CC, Tsai JD, Lin SP, et al: Galloway-Mowat syndrome: A glomeru-
lar basement membrane disorder?
Pediatr Nephrol 2001;16:653–657.
16. Srivastava T, Whiting JM, Garola RE, et al: Podocyte proteins in Gal-
loway-Mowat syndrome.
Pediatr Nephrol 2001;16:1022–1029.
17. Meyers KE, Kaplan P, Kaplan BS: Nephrotic syndrome, microcephaly,
and developmental delay: Three separate syndromes.
Am J Med Genet
1999;82:257–260.
Brief Communications 149